
MobilityWorks
Accessibility for all: Helping people connect with who and what matters most
Searching...
No results found. Please try modifying your search.
Our nonprofit can provide financial assistance through fundraising to help people living with diabetes pay for daily care and equipment.
People living with diabetes often must deal with the burden of finding diabetes financial assistance. They experience increased sugar (glucose) in their bloodstream. Causes vary by type, but whether you are living with type 1 or type 2 diabetes, your body is not correctly processing glucose. This leads to excess sugar in your body, and although glucose is an important fuel for your body’s muscle and organs, too much results in significant health care issues.
The three primary types of diabetes are as follows:
In more rare instances, individuals may develop the below types of diabetes:
Additionally, individuals can be classified as having prediabetes when blood sugar levels are higher than normal but not yet high enough to be diagnosed as diabetes. The label of prediabetes will ideally result in the delivery of patient education and corresponding lifestyle changes to help avoid the onset of diabetes.
For type 1 or type 2 diabetes, there are tests that will determine the presence of the illness very quickly. These tests include:
If type 1 diabetes is suspected, there will be a byproduct in your urine indicating that your body is not correctly utilizing glucose for energy and is developing energy from your muscle and fat tissue. With the type 1 test comes a test for autoantibodies, which are destructive immune system cells connected with type 1 diabetes.

Living with diabetes requires extreme vigilance. Maintaining a healthy diet and weight while participating in a regular exercise routine is critical for both types. Treatment for diabetes may involve insulin injections, carb counting, and frequent blood sugar checks. More advanced ways to monitor and treat diabetes include insulin pumps and CGMs (continuous glucose monitors).
CGMs serve as an alternate method to test blood glucose levels. The primary difference is that CGMs test continuously day and night, alerting a patient in real-time when levels are out-of-range. This can be especially helpful if blood sugar levels have been challenging to regulate. Although several systems are on the market, for the purpose of illustration, the Dexcom G6 model costs $6,000 per year, or $500 per month, without insurance. For a stable patient, insurance many deny coverage for a CGM as an unnecessary device.
In 2016, an artificial pancreas device system was first approved for use by T1D patients. This device, otherwise known “as a ‘closed loop system’ essentially combines a CGM, insulin pump, and glucose meter within one device and “closely mimics the glucose regulation function of a healthy pancreas.”
Although system costs vary depending on the type and manufacturer, there are also annual equipment and supply expenses. For example, “the Medtronic 670G system is between $7,000 to $8,000. But with insurance coverage, most patients pay just over $1,000 to initially get on the system, and then must pay for pump and CGM supplies on an ongoing basis. The annual cost of the CGM transmitter is $699, and sensors run from $50 to $75, depending on the amount purchased.”
According to the CDC, “diabetes is the most expensive chronic condition in our nation.”
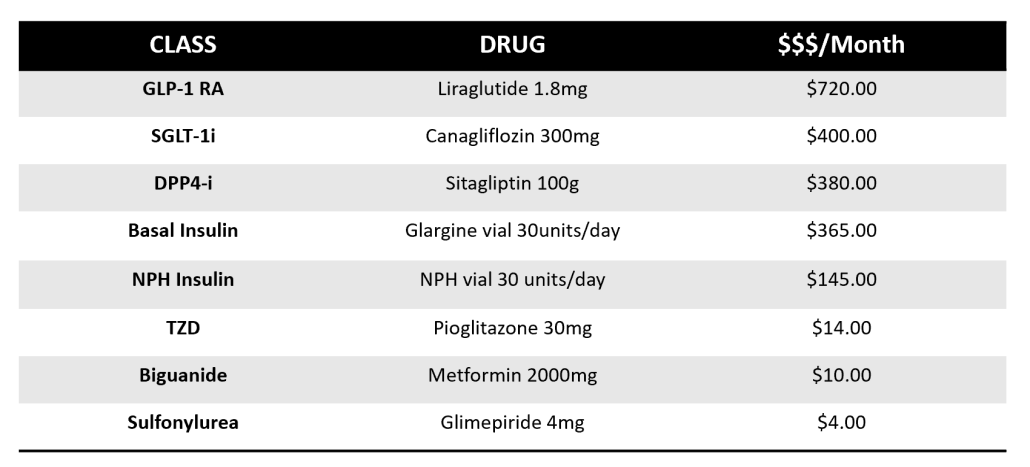
Hearing that a family member has developed diabetes can be a startling revelation. You can be overwhelmed with fear, doubt, and worry. Just remember that they’re certainly not alone – and neither are you.
While the costs associated with diabetes treatment will vary depending on situation, the expenses can be considerable. Help Hope Live is your resource for community-based fundraising to assist with the unmet medical expenses and related costs that can result from living with diabetes.
Even with health insurance, type 1 diabetes costs can be expensive. The cost of diabetes in the US in 2017 alone was $327 billion, which is up by more than $80 billion from 2012. Having additional funding can help pay for expenses that insurance may not cover. Fundraising for type 1 diabetes can be difficult but Help Hope Live’s platform was created to support financial assistance for type 1 diabetes beyond normal funding sources. Start a fundraising profile today!
Crowdfunding for type 2 diabetes can help you quickly and easily raise the money you need to pay for life-saving diabetes treatments, equipment, and supplies. Try out Help Hope Live’s medical fundraising platform to help support your financial needs for type 2 diabetes.
Establishing greater support for diabetes patients is part of Help Hope Live’s mission. Through community-based fundraising, our nonprofit organization is dedicated to helping those in need to raise funds for medical costs associated with managing daily life with diabetes and the treatment of diabetes complications.
If you need financial assistance for diabetes expenses, fundraising may be a helpful pathway. Fundraising with Help Hope Live can help you cover expenses such as:
The fundraising process with our nonprofit starts with a few simple steps:
Help Hope Live differs from GoFundMe by:
We are a nonprofit with more than four decades of fundraising experience and a 4-star Charity Navigator rating.
Here is a Help Hope Live diabetes fundraiser success story:

Help Hope Live client John Wilson received a pancreas transplant in February 2020 that cured his type 1 diabetes. He has raised over $6,000 to assist with uncovered medical expenses and sustain the gift of new life.
If you choose to fundraise with our nonprofit, here’s how the process will look:
1. APPLY for assistance
2. YOU’LL BE PAIRED with a Client Services Coordinator
3. YOUR COORDINATOR will provide you with one-on-one fundraising help, including personalized fundraising materials and guidance on how to rally your community, share your story on social media, reach out to the press, plan in-person or virtual fundraising events, and more.
Need Other Financial Help Options?
For alternatives to fundraising, you can find information on a variety of other financial assistance options. Please view our Catastrophic Illness Resource Directory for insight into sources of direct financial aid, support groups, and other resources for diabetes patients and their families.