“I am not afraid of dying, but I love living my life to the fullest.”
When we read this headline on Julie Swope’s Campaign Page, we knew we had to hear her story for our Touched by Transplant series.

When did you learn that you had pulmonary fibrosis?
On February 5, 2015, I was admitted to the hospital with pneumonia. By February 12, I was hooked up to a breathing machine and I developed an infection, which signaled a downturn for my health. In the hospital, I contracted MERSA, sepsis, double pneumonia, and acute respiratory distress syndrome (ARDS). I was placed in a medically induced coma.
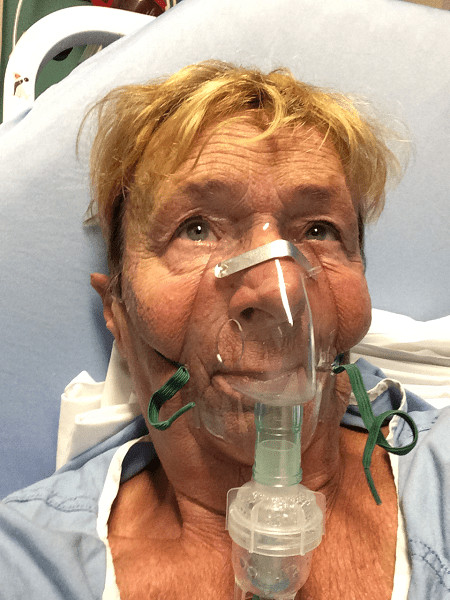
In July, I came out of the coma, and in mid-August, I returned home from the hospital with a diagnosis of pulmonary fibrosis—a lung disease that occurs when lung tissue becomes damaged and scarred. It would not be my last pulmonary fibrosis-related hospitalization.
My family was told by two facilities to put me in hospice because there was nothing they could do for me. When I was finally admitted to Hershey Medical Center, the fight began—and within two weeks, I was no longer dependent on a ventilator. I began physical rehabilitation to strengthen both my lungs and my body.
When did the idea of transplantation enter your life?
It took a long time, but in 2018, I was finally cleared for a two-week trip to Ireland. I kissed the Blarney Stone, saw the Cliffs of Mohr, and hiked extensively. Over the last two days of the trip, I began to have trouble breathing, and I needed oxygen during my connecting flight to Toronto. When I arrived there, I was taken by ambulance to the nearest hospital, where I was diagnosed with pneumonia again.
I stayed at the hospital for 16 days, then I was flown back to my hometown hospital for another 10 days. Since that time, I have been tethered to oxygen 24/7.

I read about organ transplantation as I began to research pulmonary fibrosis. I knew it was my last option if I wanted a longer and better quality of life. My goal was to work to get back to attending pulmonary rehab so that I could get stronger—ever the optimist, I believed this could happen. Every CAT scan indicated more scarring, so I started a medication in October that would help to slow the progression of the disease.
In December 2019, my doctor thought I would benefit from having a consultation about lung transplantation at Temple University Hospital. I’ve learned a lot more since that time.
How has pulmonary fibrosis affected your life?
My most treasured trait has always been my independence. Pulmonary fibrosis hit my independence with the strength of a Category 5 hurricane.

I had great physical mobility and moved freely, but now, I am tethered to an oxygen concentrator and 100 feet of plastic tubing. If I go 101 feet, I am quickly jerked back and put in my place. I have not been able to operate my business of 35 years. I’ve always been a traveler, and I can no longer travel. I used to take pleasure in watching my grandsons play soccer, but I can no longer attend these events. I used to drive everywhere, but now I must depend on others to drive me to appointments.
A tank of oxygen which used to last me three-and-a-half hours now lasts one-and-a-half. Anyone who helps me with transportation must lift those tanks in and out of the car. Sometimes, I also require a wheelchair. I hate asking for help with these things—they were never a part of my life, in which I would always be the one extending the help.
I miss the “more” that used to be in my life.
After transplant, I see myself hopping in my car whenever I want and driving to wherever I want to go. I see myself and my friends enjoying nice meals out together again. I see myself going to the Irish Festival without a wheelchair, marveling at all the progress my grandsons have made with soccer, walking up and down my stairs, and enjoying physical exercise. I see myself attending family reunions and cooking meals, and holding holiday dinners at my house again. I see myself redesigning my garden.

Has COVID-19 impacted your transplant journey?
My last appointment with my primary care physician was through video instead of in-person. I’m completing a daily symptom checklist online and taking my own temperature daily. I was told by my medical team that transplants have slowed way down overall. I imagine this pandemic will extend my waiting time for a transplant.
I think videos and phone calls for medical appointments will become much more common moving forward. If there are more public health crises like these in the future, transplantation will likely be limited during those times, creating intermittent backlogs. Organ donors will be needed more than ever.
In my community, our mayor has been providing updates on changes, and our local TV station supplies hourly updates. Several of our local churches are also providing digital services.
Me and thousands of other people have already become savvy with social distancing, but COVID-19 has introduced new fears into our lives. It has decreased the organ donor supply and increased wait times. Sometimes, a horrible thought enters my mind: What if I die before there is a match?
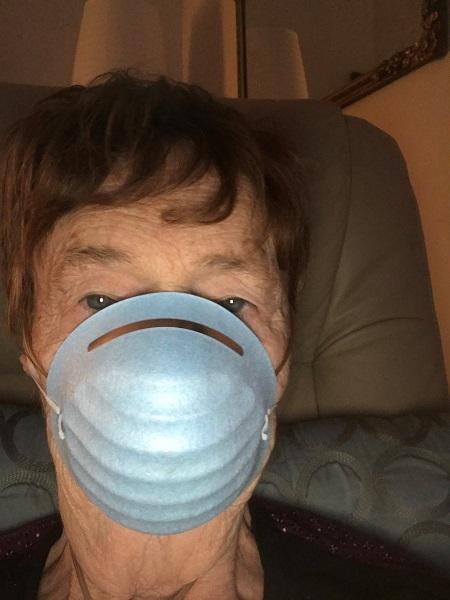
How do you find hope in your day-to-day?
I place trust in my lung transplant team, believing that if I get worse, my doctor will put me on life support until a match is found. I try to limit my exertion to try to conserve energy.
I relish the sunny days and find great comfort in nature.
It’s a wonderful time to see renewal all around us, in the spring flowers, the birds, the bees. I plan to plant some marigold seeds that I put away last year. While we can’t be outdoors in groups, we can certainly still sit on our patios and enjoy the spring.
What are your most significant health-related expenses right now?
Transportation, gas, and lodging for myself and my support system to travel back and forth to Temple Hospital (in Philadelphia) from York, PA. Home medical equipment has also been very expensive.
Messages of support on Julie's Campaign Page
What advice do you have for other transplant candidates?
Remember why you sought out transplantation in the first place: to have a better-quality life instead of just surviving. Keep this as your focus.
Keep in touch with your family and friends. If you can’t see them in person, use social media such as FaceTime, Google (Hangouts), Zoom, and other virtual and social media apps. Trust and seek comfort in your higher power.
On your Campaign Page, you mention that you are not afraid to die. Why is that?
I have lived a wonderful life, a life full of adventure, adversity, and overcoming adversity. I am my own hero. I have raised children, developed a loving support system, run a business, travelled extensively, authored books, and given much back to my community. I have made a difference in the lives of others.
The Devil isn’t going to want me, and I know why. That is why I am not afraid to die.

Julie plans to celebrate Donate Life Month by sharing this article with her local news stations to raise awareness. You can visit her Campaign Page at helphopelive.org.
Written by Emily Progin